"נאמני מרכז שניידר" הנה עמותת הידידים הפועלת למען מרכז שניידר לרפואת ילדים בישראל מאז הקמתו בשנת 1992. נאמני מרכז שניידר הוקמה במטרה לסייע לבית החולים בכל הקשור לפיתוחו ולקידומו. העמותה מסייעת לבית החולים במימון פרויקטים של בנייה, רכישת ציוד רפואי, מענקי מחקר ופרויקטים מיוחדים נוספים. עוד אודות העמותה.
הרגעים המרגשים של מפגשי המשפחות ילוו אותנו לנצח. בהסכמתן ובאדיבותן של המשפחות אנחנו משתפים אתכם בכמה מהרגעים היקרים הללו. מי יתן ונזכה לראות עוד מפגשים כאלה בקרוב 🙏🏻 תודה לארקדי דוכין שאיפשר לנו להשתמש ביצירה המדהימה שלו ותודה למשפחות היקרות.
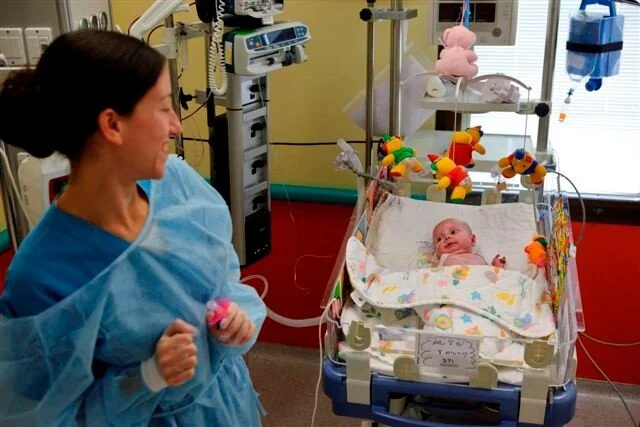
אמיליה אלוני בת ה-6 ואמה דניאל, חזרו אמש ארצה למתחם היעודי במרכז שניידר לרפואת ילדים. המפגש הראשון עם סבתא של אמיליה ועם בני המשפחה לא השאיר עין אחת יבשה.
הורים לילדים ומתבגרים הנמצאים במצוקה נפשית בעקבות המצב הביטחוני, מוזמנים ליצור קשר עם היחידה בטלפון או במייל
ההסלמה במצב הביטחוני משפיעה גם על הילדים שלנו. חלקם - מי פחות ומי יותר - חשים במתח, בדאגה ובחרדות הקיימים בסביבתם. מדובר בתחושות טבעיות, אולם ההורים חייבים לשדר ביטחון לילדיהם. טיפים ממנהל המערך הפסיכולוגי במרכז שניידר
אנחנו גאים להציג את הקמפיין החדש שלנו שנועד להשיק את בניין הזכוכית החדש, הפודקאסט הישראלי הראשון לרפואת ילדים שמיועד להורים - "ילדים זה אנחנו" ואת סדרת ההרצאות של המומחים שלנו "שניידר עד הבית"
מטרת השימוש בחדר היא לאפשר לילדים המטופלים בשניידר לבחור את הסביבה בה ייבדקו, ובניגוד לאמצעים מסיחי דעת או מפחיתי חרדה אחרים הקיימים, כגון משקפי מציאות מדומה, לשמור על קשר עין מלא עם הצוות הרפואי ובעיקר עם ההורים.
מרכז שניידר פתח ב-14 במאי 2023 את בניין הזכוכית - מגדל אשפוז נוסף הממוקם בסמוך לבניין האבן, והחל בהעברת מחלקות האשפוז.
אביתר בנאי, ישי ריבו, אמיר דדון, עקיבא, שולי רנד, אהרן ויונתן רזאל ואמנים נפלאים נוספים הופיעו בהתנדבות עם ביצועים מרגשים לשירים אותם כתבה דניאלי זוננפלד ע"ה. אנו מודים לאביה, מוטי זוננפלד, חבר ועד המנהל של נאמני מרכז שניידר, לקרן דניאלי ול-1,000 המשתתפים שמילאו את תיאטרון ירושלים והגיעו להתרגש ולתרום.
עמיחי איטליאנדר אובחן כחולה סיסטיק פיברוזיס לפני כ-19 שנה. למרות המחלה, עמיחי מתכוון לרוץ במרתון תל אביב, בפברואר הקרוב.
נאמני מרכז שניידר מרכינים ראש על פטירתה של גברת אורה הרצוג ז"ל. אורה כיהנה כנשיאה הראשונה של ״נאמני מרכז שניידר״ (בשמה קודם: ״המועצה הציבורית למען המרכז הרפואי לילדים בישראל״), והיתה מהדמויות המשמעותיות שהובילו לפתיחתו של מרכז שניידר לרפואת ילדים בישראל.
מרכז שניידר לרפואת ילדים בישראל חגג 30 שנים של מצוינות ואנושיות באירוע יוקרתי ומרגש. האירוע התקיים ב 13/12/21 במלון הילטון בתל אביב במעמד נשיא המדינה מר יצחק הרצוג ורעייתו מיכל, בנוכחות שר הבריאות מר ניצן הורוביץ, ובהשתתפות מאות ידידות, ידידים ואנשי צוות.
לכבוד בת המצווה שלה, ביקשה מיה ממשפחתה וחבריהם לתרום כסף עבור המכון לרפואת ריאות במרכז שניידר לרפואת ילדים בישראל, זאת במקום לקבל מתנות לבת המצווה.
לכבוד יום הולדתה ה-10, אלה השלימה מבצע התרמה שהיא יזמה והוציאה לפועל בעצמה. היא הצליחה לגייס תרומות לרכישת מכונת הנשמה עבור מחלקת הפגים של מרכז שניידר לרפואת ילדים בישראל.
האחות רויטל צ'רניאק זכתה השנה במלגה ע״ש ציפי דנה. הפרס הוענק לה בטקס חגיגי במרכז שניידר לרפואת ילדים בישראל.
טקס הוקרה ופרידה מנשיא העמותה, ישראל מקוב, ומיו"ר העמותה, רונן טוב, התקיים במרכז שניידר לרפואת ילדים בישראל.
מפגש מרגש בין משפחת פוקס לבין צוות המחלקה לרפואה פסיכולוגית - בתם רומי פוקס טופלה בשניידר מספר שנים, התקיים היום במרכז שניידר לרפואת ילדים.
במבצע מורכב שארך כ-10 שעות, העבירו אתמול הצוותים הרפואיים במרכז שניידר לרפואת ילדים, את הילדים המאושפזים במצב קשה למתחם חירום ממוגן בבית החולים.
הניסוי של מרכז שניידר לרפואת ילדים נבחר להשתתף במשימת רקיע של איתן סטיבה, הישראלי השני בחלל. ניסוי זה בודק את קצב גידול .התאים הסרטניים, בארץ לעומת בחלל - בהיעדר כוח הכבידה. משימת רקיע יצאה לדרך בהובלת קרן רמון ומשרד המדע והטכנולוגיה
כבר כשהייתה בת ארבעה ימים התגלה גידול על כף רגלה של רומי פוגל. כשהתברר שהוא סרטני, אמה נחרדה מהמחשבה שבתה תצטרך לעבור כימותרפיה בגילה הרך. למרבה המזל, המרכז הרפואי שניידר נכנס בדיוק באותה עת לניסוי של תרופה ביולוגית חדשנית, אשר נלקחת כסירופ דרך הפה. הגידול הצטמצם, נכרת, ומהטראומה נותרה רק צלקת קטנטנה
קרן המלגות ע"ש רחלי בצלאל הוקמה בעקבות זיקתה של רחלי לתחומי המחקר. הוריה החליטו להנציח את זכרה באמצעות הענקת מענק מחקר שנתי לנבחר/ת המחלקה ההמטו-אונקולוגית העוסק/ת במחקר יישומי בתחום מחלת הסרטן בילדים.
בתקופת משבר הקורונה, כשהמירוץ המטורף של העשייה נעצר, ישבו שירלי ואורית וחשבו איך לנצל את הזמן הפנוי ולעשות משהו טוב.
ד"ר ברון-הרלב מחליפה בתפקיד את פרופ' יוסף פרס, אשר שימש כמנהל מרכז שניידר בשתיים עשרה השנים האחרונות ופורש לגמלאות
הילה יהודה, מתנדבת בנאמני מרכז שניידר ועובדת בחברת מיקרוסופט, החליטה לארגן פרויקט מיוחד לטובת ילדי שניידר – לרתום את חבריה לעבודה לפרויקט מימון המונים שכולו קודש למען מטרה חברתית.
המערך ההמטולוגי-אונקולוגי במרכז שניידר השיק לאחרונה את פעילות "צוות דניאלי" לזכרה של דניאל זוננפלד ע"ה, בת שירות לאומי שעבדה במחלקה במסירות רבה.
בני משפחת אריסון ונציגי קרן אריסון הגיעו לביקור במרכז שניידר, שבמהלכו התקיים טקס הסרת הלוט מעל שלט הנצחה לקרן אריסון, שנקבע בקיר היחידה לטיפול נמרץ לב.
בערב השתתפו כ-900 תורמות ותורמים. את הערב הנחה בכישרון רב יאיר ניצני, על הקייטרינג המשובח ניצח איתמר פרץ, ולהקת תיסלם האגדית הקפיצה את הקהל בהופעה בלתי נשכחת.


מגדל אשפוז חדש